Kids & Post-Covid Conditions
Several studies show that long-term symptoms can occur in children and adolescents.
The United Kingdom Office for National Statistics estimates:
– 12.9% of children 2 to 11 years of age
– 14.5% of children 12 to 16 years of age
still experienced symptoms 5 weeks after infection.
WARNING: From the CDC
Contact your child’s doctor, nurse, or clinic right away if your child is showing symptoms of MIS-C.
Multisystem inflammatory syndrome in children (MIS-C) is a serious condition associated with COVID-19 where different body parts can become inflamed.
– Ongoing fever PLUS more than one of the following:
– Stomach pain
– Bloodshot eyes
– Diarrhea
– Dizziness or lightheadedness (signs of low blood pressure)
– Skin rash
– Vomiting
Be aware that not all children will have all the same symptoms.
All patients who test positive for a SARS-CoV-2 infection should have at least one follow-up conversation or visit with their primary care medical home.
– The American Academy of Pediatrics
Guidance from The American Academy of Pediatrics
All patients who test positive for a SARS-CoV-2 infection should have at least one follow-up appointment with emphasis on cardiac symptoms
In-person visit:
• Patients with moderate or severe acute infection*
– AND –
• Patients with lingering symptoms regardless of acute infection severity
Telehealth:
• Asymptomatic or mild cases that no longer show signs or symptoms
*Moderate or severe acute infection is defined as >4 days of fever, chills, body pain, lethargy.
What is Long Covid?
Long Covid is defined as ongoing, newly acquired health problems experienced after having COVID-19. Some people recover, while others experience chronic illness.
Identifying Long Covid in Children
Know the Signs
Signs and symptoms of Long Covid overlap with many other conditions and always warrant an appointment with your child’s pediatrician.
- Cognitive symptoms such as confusion, difficulty retrieving words, poor working memory, spatial instability, and disorientation
- Suddenly performing poorly at school
- New struggles to pay attention
- New struggles to finish school work
- Sensitivity to light, sound or vibration, taste, odor or touch
- The inability to be upright. See: Orthostatic intolerance
- Becoming out of breath with minimal activity
- Complaining of racing, past, or pounding heart
- Saying “I don’t feel good” for an extended period of time
- Complaining of exhaustion
- Becoming fatigued quickly
- Sitting while other kids are playing
- Regularly sitting with their legs under their body (naturally compresses and raises blood pressure and “feels better”)
- Complaining of headaches, dizziness, or body pain
- Poor temperature regulation, cold or heat intolerance
- Worsening of symptoms after any mental, emotional, or physical activity sometimes delayed by hours or days. See: Post Exertional Malaise
- Muscle fatiguability, weakness and fasciculation; poor coordination and ataxia
- Pain in the muscles and joints
- Immune symptoms such as tender lymph nodes, recurrent sore throats, fevers, or flu-like symptoms, and new food or chemical sensitivities
- Headaches of a new type, pattern, or severity
- Gastrointestinal symptoms such as nausea or abdominal pain
- Increase in allergy, rashes, or signs of inflammation
People who test positive for SARS-CoV-2 should not exercise until they are cleared by a physician.
– The American Academy of Pediatrics
WORK WITH YOUR DOCTOR
We want to stress the importance of exploring other possible conditions and causes of symptoms with your child’s care team. The Centers for Disease Control & Prevention and The American Academy of Pediatrics has information for doctors on the assessment, evaluation, and testing for patients with Long Covid symptoms.
Doctor assessment for Long Covid >

Parents Say
“He is not as active as he used to be… he stopped playing.”
“Her headache would not go away.”
“She never got well after we had Covid, and then new symptoms started to develop weeks after.”
“He has reoccurring fevers almost daily.”
“She has constant joint and back pain.”
“Any time we go and do something, the next day they are sick.”

Kids Say
“I don’t feel good”
“My body hurts”
“I am really tired again”
“I can’t run like I used to.”
“My legs are so heavy.”
“My heart is pounding.”
“My legs are wobbly.”

Common Symptoms
• Severe exhaustion and / or weakness
• Headaches
• Stomach pain
• Body pain, tingling, pins and needles
• “Brain Fog” – loss of words, inability to concentrate
• Shortness of breath and / or wheezing
• Light & sound sensitivity
• Low blood pressure and / or high heart rate
• Fainting
• Internal vibrations, shaking
• Rashes, itching, red eyes
• Inflammation
• Heart Palpitations
• Reoccurring fevers
• Nausea
• Weakness
• Sore throat and / or sniffles
• General sense of being “unwell”

Acquired Syndromes
CDC Recognized
• Myalgic encephalomyelitis (ME/CFS)
• Fibromyalgia
• Post-treatment Lyme disease syndrome
• Dysautonomia and Orthostatic Intolerance (OI)
– POTS (heart rate increases on standing)
– Orthostatic Hypotension (blood pressure drops on standing.)
• Mast Cell Activation Syndrome (MCAS)
Patient Observations
• Small Fiber Neuropathy
• Hypermobile Ehlers Danlos Syndrome (hEDS) or Hypermobility Spectrum Disorder (HSD)*
*Life-long but often unidentified
See Your Pediatrician
The in person follow-up assessment for those with moderate or severe cases and those with lingering symptoms should include the American Heart Association 14-element screening evaluation with special emphasis on cardiac symptoms including:
• Complete physical examination
• Chest pain
• Shortness of breath out of proportion for upper respiratory tract infection
• New-onset palpitations
• Syncope
• Complete physical examination
• EKG
SEE YOUR DOCTOR
Any child or adolescent who reports these signs/symptoms should have an in-office visit that includes a complete physical examination, and consideration for an EKG should be given prior to clearance to return to physical activity.
Support for Daily Living
Identify all necessary supports to facilitate return to activities of daily living (including return to learning, play, and employment.) This may include:
- Gradual return to school and cognitive activities based on tolerance
- Cognitive “rest periods” throughout the school day
- Interval academic accommodations
- Close monitoring and communication by the family, school, and pediatrician to assess progress
- Other academic adjustments or accommodations as needed.
Keep a Symptom Journal
Symptom journals can help keep track of your child’s complaints, frequency, intensity, what makes symptoms better, and what makes them worse. With the nature of Long Covid, it is important to include activity tracking as well to identify post-exertional malaise.
DOWNLOAD OUR SYMPTOM & ACTIVITY TRACKER >

Accommodations in School
Schools are required by law to provide reasonable accommodations and modifications to students who have disabilities. Learn about ways for helping children with Long Covid succeed in school.
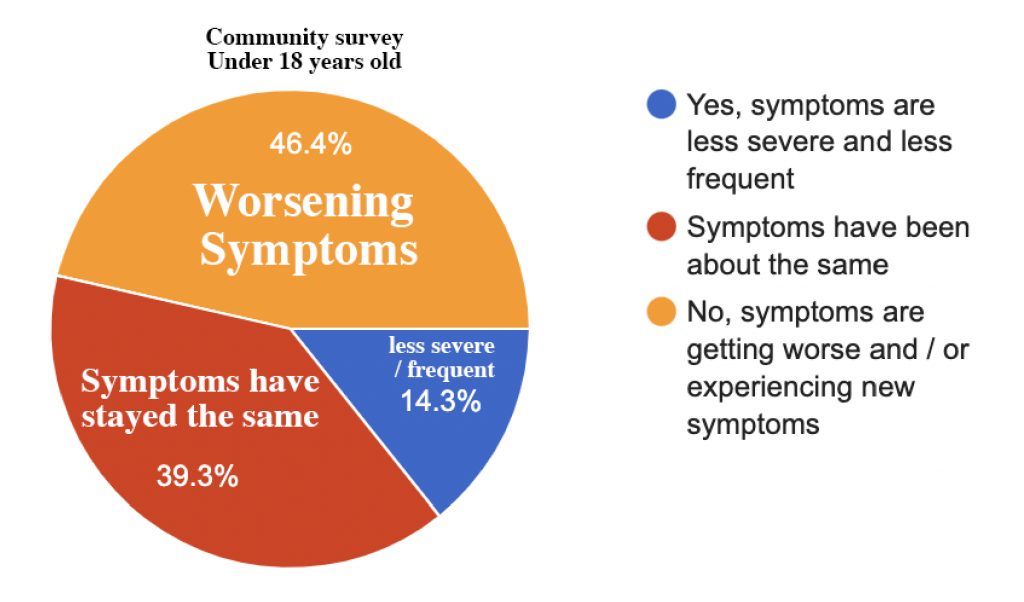
2021 Caregiver Survey
Our Long Covid caregiver survey reported that 46% of those with Long Covid experience a worsening of symptoms or new symptoms more than 6 months after the initial illness.
We speculate that this may in part be due to the delay in recognition and ineffective treatment / symptom management. It is our hope that early recognition and symptom management results in better outcomes in the future.
It is extremely important to encourage your child to rest and not “push through” symptoms if they are experiencing Post Exertional Malaise.
December 2021

Long Hauler Stories
Read first hand experiences from those impacted by Long Covid and Post Covid Conditions.

Find a Doctor
Long Covid Families has asked caregivers to share any doctors who have been helpful for treating Long Covid symptoms in with their child. Additionally, we have a list of Long Covid Clinics currently taking pediatric cases.

Symptom & Activity Journal
Keeping track of symptoms, their severity, and activities can help you identify trends in you or your loved one’s health to facilitate conversations with your doctor.

Daily Living
Long Covid Families is dedicated to helping caregivers, children, and individuals find practical ways to improve their quality of life despite the impact of chronic illness.

Connect with Us
Join our group for support.
You can find us on Facebook at Long Covid Families.
COMMUNITY SUPPORT
Long Covid Families is happy to support the community in any way we can. Join our Facebook Support Group, follow us on social media, or contact us, anytime.
SUPPORT THE CAUSE
Donations are tax deducible and every little bit helps us pay for the essential tools we use for advocacy & awareness. Donate to Long Covid Families.