Settling into chronic illness
In March 2021, four months into my illness, I was still playing baseball with my boys in the yard. It was my youngest first go at t-ball and we wanted to help him get the gist. I could run the bases. I could hit the ball and get fake home runs against my all star teen. This feels like another life now.
Each decline has caught me totally off-guard, and to be honest, I have no idea how I got here. A feature of my illness can be memory loss and “brain fog” but maybe I was just way too busy to notice what was happening? Or more likely, I didn’t see the magnitude in each milestone.
This is me, trying to figure out what exactly happened.

In the beginning
When I first got sick with COVID in November 2020, my biggest issues were dizziness and every once in a while, a heavy wave of exhaustion that would stop me in my tracks. I also had hives and wheezing, but medication made these almost non-existent.
This all was disruptive and concerning, but I was seeing doctors, figuring out what was happening. I had hope, a string of bad days and a string of good days. I didn’t feel great, but I was pushing through it for the most part.
I was busy
I continued to work full-time, remotely, in a somewhat stressful fast-paced job. Physical therapy helped my body pain at 8am on Tuesdays. I was cyber schooling both of my sons due to COVID, though the older one rarely accepted any help. And I ran a little Etsy store for the jewelry I was making. It was a hobby that had really taken off and I was shipping a handful of orders each week.
The kids also kept me busy. My older son also had baseball a few times a week. He was on a travel ball team in addition to our local seasonal teams and all star team. My younger son had just started T-ball and swim lessons, physical and occupational therapy all multiple times a week.
It was a lot.
My husband and I divided and conquered. I figured we could make it work for a while, and we did.
I had thought that even though my symptoms were still there at times, I had mostly recovered and could learn to manage the bad days.
The first collapse
On April 14th 2021, I had taken my nightly hot bath and when I got out, I collapsed with dizziness.
This is my first sudden blackout at home.
The doctors had forced me to blackout in the hospital in the beginning of March with the tilt table test. They strapped me to a bed and stood me up to a standing position to watch my vitals and document why I was getting dizziness on standing. I was diagnosed with Orthostatic Hypotension, meaning my blood pressure was suddenly dropping to dangerously low levels, hence the black out. But we didn’t know why, though there was theories, there was also a handful of diseases to rule out.
This first episode at home was concerning. I was surprised and scared.
I continued to feel awful, getting dizzy any time I bent down. It was at this time I decided I needed to stop selling on my Etsy store.

🚩OH SHIT MOMENT #1
This was the first time I really started to freak out. I wrote my neurologist because she was booked until September. How was she going to fix me if I had to wait 4 months? I couldn’t go on like this — I thought.
At this point, the neurologist started calling me a Long Hauler, so I asked for a referral to the COVID Clinic.
Second recovery
By the beginning of June 2021, I started having good days again. I was 7 months into my illness and it was a miracle, I was healed! (Seriously, I finally told my story on Facebook and claimed I was all good!)
I was still undergoing testing, but I felt mostly okay. More good days than bad suddenly.
Things got warm
It wasn’t long before I realized sitting in the sun at my son’s baseball games was no longer an option. The heat made me unbelievably nauseous and dizzy.
But I adapted. I sat in the shade, started bringing a wet neck towel, and wearing compression gear under a long skirt.
It helped some.
I also had to use this method for some of my activities at home. Like going in the garden, or hanging out with my little by the sandbox.
Nervous about functioning
We had planned a vacation with my husbands family to the great Smokey Mountains — Tennessee mid-July 2021. The average temperature for this time of year is 89* Fahrenheit.
This all sounded not doable for multiple reasons. But I would have to figure it out.
The family would want to sight see and shop. What would they think of me if I have to keep sitting, or hang back at the house most of the time?
The heat induced dizziness, and nausea made it feel like a disaster waiting to happen.
A little hotter
In the final hour, two weeks before our trip, our cabin CAUGHT FIRE. 🔥 Literally.
I felt awful for my mother-in-law who had been planning the trip for a year. But it ended up being a true blessing for me when instead we planned our trip to Lake Erie.
During our stay, the weather was actually much cooler than at home and I felt WONDERFUL!
I still had difficulty waking up in the morning and I was keeping an eye on my blood pressure, but I was able to play with the kids, pretend I’m a photographer, help out with the house, and I functioned almost completely normally.
We took a day and went to a local amusement park. I rode rides and walked for hours… and was totally fine.
This was perplexing. Was I really so dizzy and tired at home? I didn’t understand. Maybe I was being dramatic.

COVID Clinic — month 8
During my Erie vacation I had my first tele-health appointment with the covid clinic. This doctor was wonderful. I had told her about my journey and testing and she validated that my experience was very much like many of her patients.
She referred me to cognitive therapy for brain fog (it’s like your train of thought suddenly hits a wall and there’s NOTHING) and a rehab center for exercise intolerance because I was short of breath often.
The doctor gave me the names of a few cardiologist who were interested in working with Long Haulers and advised me to finish up my testing with endocrinology to rule out salt wasting diseases.
🚩OH SHIT MOMENT #2
The doctor was clear — she did not expect this treatment to help and told me she would be talking to me again soon, even though we had nothing scheduled.
That was a bit concerning.
Rehab program
I had already been working with my normal physical therapist on low impact strengthening exercises to tighten up the muscles around my loose joints. My body pain had gone from a 7 to typically none or a 1. He was amazing and I trusted him.
But none the less, I figured I would let this rehab physical therapist evaluate me. They did a battery of tests, most of which were normal with the exception of muscle weakness, some dizziness when I closed my eyes and turned my head while walking.
The evaluator decided that since we did not replicate the shortness or breath or dizziness, there wasn’t much to do for me.
When she said that Orthostatic Hypotension is more cause by lifestyle choices… I knew I wasn’t going back.
A large loss — month 9
On Sunday August 1st, my family woke up early and went to my older sons playoff game for the Little League World Series.
Not long into the game, my husband got a call that one of our close friends had passed away. I didn’t take it well in the middle of the baseball moms.
That evening, I gathered with old friends. The next morning I woke with a sore throat. SHIT. Had I caught COVID again?!
All day on-and-off I had chills. My heart rate kept elevating into the 150’s which would make me light-headed. I was convinced I had a bug.
I was so cold, I laid in the grass next to my son’s sandbox in the sun. I figured the Vitamin D would help, that was a rumor in the beginning of the pandemic.
Man down
But when I got too warm and went to move, I started to black out and fell over. I tried to crawl a few feet, and just went back down, over and over.
I needed to get back in the AC and desperately wanted to make it to my blood pressure machine to see what was happening. Low readings were sent to my Neurologist for months but since it was a wrist Blood Pressure machine she didn’t feel they were accurate.
Then I finally had purchased a fancy, FDA approved, Bluetooth enabled arm cuff.
After about 5 minutes of starting and stopping I finally made it inside. I pushed and pushed and after probably another 5–10 minutes I somehow got to my Blood Pressure cuff.
(Note: my husband was with me and witnessed this but I didn’t ask him to get the blood pressure machine or to try to get me inside. I’m just not used to asking for help. And really I hate asking.)
As I stood taking my BP, I lost both my vision and hearing, but I caught the reading: 76/46 with my heart pounding at 150 beats per-minute, frantically trying to bring my blood pressure up.

The next few days I was very sick. The sore throat and chills continued but I had no fever. I was dizzy any time I walked, often gracefully collapsing before the blackness totally overtook my sight. Bending was out of the question.
🚩OH SHIT MOMENT #3
Feeling hopeless, I wrote both my neurologist and the COVID clinic doctor. To my surprise, the my neurologists response brought me even lower.
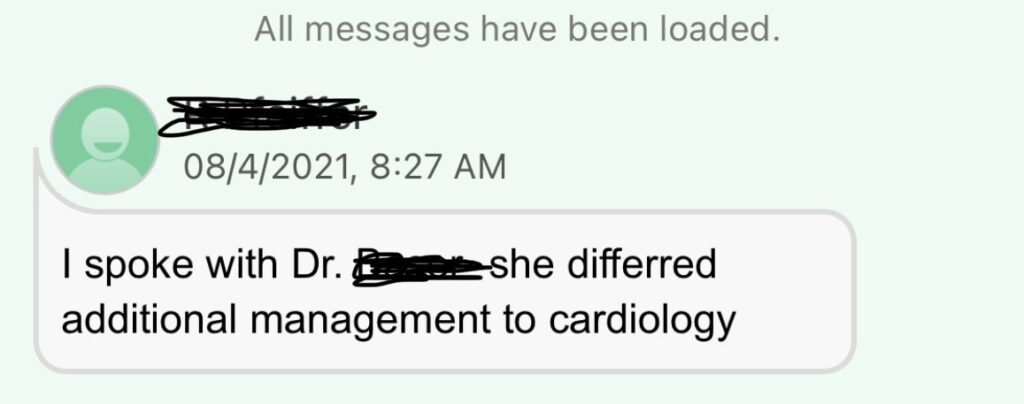
Was she breaking up with me?
I didn’t yet have an appointment with cardiology but I suppose I better hurry and get one.
The COVID clinic doctor called me on a Friday evening in response to my message. I was impressed. She would pull some strings and get me in with cardiology and a well respected allergist as soon as possible. While I waited, she prescribed the most common medication used for Orthostatic Hypotension, Midodrine.
I forced myself to go get a COVID test at a drive through facility. Thankfully negative.
At my friends funeral. I sat in the grass as my friends stood around talking. During the service, my husband brought me a chair so I could sit in the back. Standing was difficult.
I skipped 2 weeks of physical therapy appointments, I was too sick. But I continued to work remotely, although sometimes having a delayed start since it became impossible to wake up in the morning.
Get it girl — month 9
Once I finally started having some good days again, I got to the pharmacy to pick up my new medication.
I started the new med and went to my physical therapist. Him and I dove into current COVID rehab methods. We did my normal strengthening and added breathing exercises laying on the floor.
We decided to try 6 minutes on the exercise bike, taking my BP before and after each session.
I had been doing the stepper for 5 minutes with no problem as a warm up since I started there in the spring, and we did not expect for me to have any issues with the bike.
Around 5pm that night, I started to feel extremely sick again. Chills, increasingly dizziness, and once again had a sore throat. I was exhausted. I remember driving my son home from his own physical therapy, nervous I was going to fall asleep while driving.
The next day I woke up with painful ulcers under my tongue and down my throat. An allergic reaction to the Midodrine which I never took again.
I called my doctors, and they said to up my antihistamines and go to the ER my wheezing got any worse than normal. Gargling with Pepto helped the pain. It was 4 days before I was better… again, I continued to work remotely. Suddenly started to feel better day 5.
And she’s up!
By my weekly physical therapy appointment I was once again almost better. I updated him on the week and mentioned my concern about the bike being too much, but couldn’t say for sure if it was the bike or the allergic reaction, so we tried again.
Again, that night around 5pm on the way home from my son’s appointment, I was struggling to stay awake. It was the middle of summer, bright as day, a warm and beautiful evening… and this was down right bizarre.
More concerning another new symptom showed up, which really made me nervous.
I was sitting outside doing some work when my hands started shaking. Like a tremor. It resolved within about 30 min. I video recorded it. And decided to ignore it. Maybe I just needed to eat. I ate and it went away, but later that day it returned. And the next day.
Scaling it back
At physical therapy we decided to not proceed with the bike and to try the stepper machine instead since I had been fine with doing 5 minutes on it for months. We would increase the distance little by little each time. This seemed to work MUCH better, for about 3 weeks…
A sharp decline
Now it was into October, month 11, and I had recently collapsed without my husband home.
My kids were so used to seeing me randomly collapsing that no one even noticed anymore. I would lay on the floor and wait. Wait for my vision and hearing to return. Wait for my chest to stop pounding out of my chest.
🚩OH SHIT MOMENT #4
This “flare” just wasn’t getting better. And the new symptoms were scary.
I was waking with my face completely swollen. Sometimes a droopy eyelid. I was suddenly missing words and names of common people and common objects. And what is this tremor about? Did I have MS? Parkinsons? Brain lesions? (All of which have since been ruled out.)
I started randomly getting STABBING nerve pain in my fingers and toes with an alarming intensity. Thankfully it was brief and would come in waves only lasting around a minute.
I was still doing cardio at physical therapy and once I got to a certain intensity using the stepper, I started experiencing the “crash” again, each time about 8 hours after my appointments.
🚩OH SHIT MOMENT #5
By now, I wasn’t recovering to the state I once was.
Places to be, things to do
My older son was taking a girl to the Home Coming Dance for the very first time and I was so excited to help pick out his suit and take pictures of the teens, but I was having issues walking around the house without collapsing and blacking out.
I felt fine sitting in the car on the way there, and I just couldn’t picture me walking into the store, looking perfectly normal- fit and in my 30’s, and grabbing a wheel chair. Then having to ask my husband and son to push me.
Our trip was mortifying for me. Even though I had planned to use the wheelchair, even calling ahead before we went, I didn’t. I had to sit repeatedly on the ground, in public. With my husband and my kids just looking at me. Strangers looking at me. And I wasn’t quite sure how I was going to make it out of the store.
That experience humbled me.
Disability is not a dirty word
We got a push wheelchair for me from a local church. I promised them that I intended on getting better and returning it. I told my PCP about the ordeal and asked for a prescription for a power wheelchair so that I at least didn’t have to have someone push me, and maybe I could go to the store on my own even. But she deferred to the cardiologist.
The cardiologist put me on a new med, Fludrocortisone, and said he wanted me in the physical rehab they would prescribe the wheelchair.
And the physical therapist, who had watched me do the bike and the stepper with no issues — aside from off the wall BP and Heart Rate readings — just didn’t understand. He wasn’t seeing my collapsing, and he wasn’t in my body to know what it feels like.
He told me he understood why I wanted it. But I was young and he didn’t want me to have to rely on it. This was my first taste learning about the way our society thinks of disability.
I told him clearly that my blood pressure drops to 70/40… there is not blood in my brain and this is dangerous. It increases risk of stroke.
He was sorry, but it wasn’t happening. He suggested a scooter…

Am I gonna die?
All of this sent me into my typical research spiral mode which uncovered a long term study of middle aged people with Orthostatic Hypotension (OH.)
🚩 OH SHIT MOMENT #6
The American Academy of Neurology published a study in 2015 titled Clinical implications of delayed orthostatic hypotension: A 10-year follow-up study by: Christopher H. Gibbons, MD Roy Freeman, MD. The researchers found that middle aged patients with Orthostatic Hypotension, had a 10-year mortality rate of 64%.
It is only one study… but it scared me to my core.
I sat on it
I sat on my new findings for a while. I told my husband three days later but he didn’t say much. About a week later I told my best friend at work but again, she wasn’t sure what to say.
But no one seemed to understand even though I know they cared.
Worse yet my doctors kept calling my condition POTS, (which is a related condition, but to my knowledge not as serious and not as life threatening.) So without a medical professional to discuss this with, I really still have never figured out what to make of it.
And again, life continued.
But actually, I didn’t sit
Homecoming
I day of the of homecoming I woke up feeling well, excited! Went to the flower shop and then the grocery store. It took a bit longer than expected and I found myself sitting on the ground twice due to dizziness. Alone with my 6 year old. But it was a big day, and I persisted.
I used my fancy camera and took pictures of all the kids for homecoming… until I suddenly crashed. “It’s time to go,” I told my husband. But I couldn’t think. I didn’t know what to tell the other parents. I would grab a few things and then sit, grab some more things and sit some more. My brain wasn’t working, I couldn’t remember any of their names.
🚩 OH SHIT MOMENT #7
When I finally got to the car I put my chair back and settled into what felt like a form or paralysis. I couldn’t make words. I couldn’t move. When we got home, I was able to get in the house and go straight to bed.
A few days of extra dizziness paying for my actions, and I recovered some.
Halloween
I knew better than to walk for trick-or-treat… but again — how the hell are these people going to push me around?
I brought the wheel chair and again lost my nerve to use it, but this time I didn’t collapse. I had never felt so grateful. Grateful to be walking. Watching my babies do their thing. I was in heaven.
Since we were able to keep moving, I believe the pumping of my legs and keep my blood pressure up. Though, it didn’t really matter. An hour of walking was too much and I would pay.

🚩 OH SHIT MOMENT #8
When I got home I settled into a chair while my kids sorted and traded their candy. The exhaustion waved over me. My head became 500lbs. I remember my son looking at me and talking, and I couldn’t answer him. I knew I wanted to. But everything felt slow and heavy. All I could get out was stare and mutter, “One Minute.”
This was the second time this had happened, and though close to inexplainable, it caught my attention.
Connecting the dots — 1 year anniversary
The only understanding I really received was from fellow patients.
Without them, I would be so lost. They knew the correct names for disorders, what tests to ask for. They knew lifestyle changes that make things better, and activities that make things worse.
The exercise and activities making me worse ended up having a name. Post Exertional Malaise. And this was something that happens with people who have chronic fatigue syndrome or myalgic encephalomyelitis, ME/CFS.
🚩OH SHIT MOMENT #9
The reading on ME/CFS: 75% are unable to work and there’s only a 5% recovery rate… was a little bit grim.
I found out there were people who have been sick for decades without any type of useful treatment. But it wasn’t until I watch the 2017 film UNREST by Jennifer Brea on Netflix that everything really sunk in.
These people had all of my symptoms.
✔️Typical onset was a viral infection.
✔️ Blood pressure drops & dizziness.
✔️ Crashing paralyzing fatigue. Sometimes unable to move or talk.
Even the other diagnosis I gathered since having COVID, have a high rate of prevalence with ME/CFS: Hypermobility Spectrum Disorder & Mast Cell Activation disorder. For so many of these people they have the diagnosis soup. A cluster of common occurrences… that’s really hard to sort out why and how is causing what.
It wasn’t until I saw these people suffering that I actually understood why I can’t keep pushing.
I watched, and I sobbed.
WHY, HOW WAS DOCTORS NOT TELLING ME THIS?!
I learned as much about ME/CFS as I could. And quickly found its controversial history. Despite being classified as a neurological disorder back in the 1950’s, by the World Health Organization. The CDC and National Institute of Health had been working with patient advocates for decades, but still there is hardly any funding into ME/CFS research.
It’s not taught in medical schools and many medical professionals don’t know much about it. The majority still seem to have reservations about its validity despite our government guidance for diagnosis and “treatment.”
Progression
I found out that people usually progress due to the crash cycle. Some simply never recover after their crash. Most concerning to me was the statistics widely sited that about 25% of people with ME/CFS are house bound or bedbound.
The worse cases have constant disabling symptoms and spend their days in a dark & quiet room, some unable to speak, and some with a feeding tube as they are no longer able to eat.
Rest to recover
I took to my Long Covid support group to learn more and found person who swore that they got better by taking off of work for 2 months and doing absolutely nothing.
Is this something I could even do? I wasn’t sure. After talking to my partner in crime at work, we decided that at the very least I could take a 2 week vacation and see if it helps.
A day before my vacation, during my lunch break on November 18th, a year to the day of us getting COVID… I watched a webinar with a director of the National Institute of Health explaining Long Covid and the overlap with ME/CFS.
To say I was in shock was an understatement.
A new approach
I took two weeks off of work over thanksgiving break. I had no idea how active I was until I tried to stop. By day 10 I was finally adapting to my couch, closing my computer, watching movies, starting to relax.
A few days after that, I got up to go to the bathroom and collapsed. The panic you feel when your nervous system is failing is enough to scare you into compliance with whatever your body wants.
I knew this wasn’t okay and I cannot keep doing this. I needed to REALLY, actually, STOP and TRY to do nothing.

This utter panic forced me to called and apply for short-term disability without knowing if I would be approved or not. I set up a meeting with my boss, director, and partner in crime.
I told them some details of what I have been facing, how I have been getting worse, and that this was my Hail Mary. The only approved “treatment” for post-viral illness.
Again, I sobbed. And I wasn’t the only one.
I knew I loved my work. But I never really realized how MUCH I love my work. How much self value I gained by being able to do my work, and do it well. And the sheer terror that I am not long able to do my work and be healthy.
Am I alive? — month 15
December and January have been a blur. I continue to see doctors, do therapies, run tests, find new problems. But at a slower rate.
I would love to say that I have been feeling better or at least stabilizing. I did think that for about two weeks thanks to a new medication that has really helped ease the dizziness.
It seems like my good days are a bit better now with the medication, cromolyn sodium, and I am very grateful… but my bad days are getting worse. Christmas Day I started migraines with light and sound sensitivity.
In trying to quantify my very personal experience I found a few different ways to measure disability from post-viral illness:
Bell CFIDS disability scale
🚩 OH SHIT MOMENT #10
Now, I am go between a 30–20 on the Bell CFIDS Disability Scale
30: Moderate to severe symptoms at rest. Severe symptoms with any exercise; overall activity level reduced to 50% of expected. Usually confined to house. Unable to perform any strenuous tasks. Able to perform desk work 2–3 hours a day, but requires rest periods.
20: Moderate to severe symptoms at rest. Unable to perform strenuous activity; overall activity 30%-50% of expected. Unable to leave house except rarely; confined to bed most of day; unable to concentrate for more than 1 hour a day.
I have progressed to experiencing crashes if I do more than 2 hours on the computer or on the phone at a time. Meaning 1 hour of computer and 1 hour on the phone is my limit for each day.
The crashes are getting harder. My cognitive function is getting worse.
More recently I am unable to bring my heart rate down and my blood oxygen levels are also going down to 94 for extended periods. In this case, I take the advice of my online friends and get into bed with a weighted blanket and try to sleep it off, which seems to take hours.
I am able to drive my son to baseball practice. I can even be able to run into a store quickly to grab something. But I am not able to stay out in public, even sitting, for very long without crashing for days. (Think funeral home.)
Cue existential crisis
I have spend a good part of the last 3 months pondering big questions.
Ideas like — what is my value? If I cannot do much for people, and I cannot do much for myself, what do I bring to the table and who am I?
I’m not sure if I will qualify for long term disability, so maybe I do have to work until I am unable to move, speak, or eat because we need my income, or some income from me for my family to survive. Or maybe I will qualify for disability and keep declining anyways. In which case I started preparing documentation for my husband.
My biggest concern right now (besides not losing the house and being able to feed the kids) is if I do become bed-bound, can I get my husband some help? Is there programs that can potentially take care of me or even help with house work? Would I have enough friends that everyone could come be with me one time a month? Would they?
I still struggle with would I want him even stay with me? Having the kids have to see me like that. Being an anchor pulling them down. No family vacations. No trips. It’s hard to imagine.
And then I guess I realize I’m already mostly there.
I was invited to my cousins wedding out of town. This cousin sang in my wedding. I know I shouldn’t go, not unless I am able to do these little things without crashing. But no one even understands just how sick I am. I just don’t know how to live like this yet.
I started to mourn who I was, and love who I was, miss who I was. I made tribute videos to my old life. It sounds weird, but it really helped. There is a lot of fear that I will never be that independent and capable person again.
When in doubt, sit
I have found ways to adapt and methods for taking care of myself. I am adapting to the new version of me, I just need everyone else to catch up.



I am nowhere, and I am here
One of the hardest things is the lack of acknowledgement.
Don’t get me wrong, I have people who love me, check in on me, and some even let me talk in circles about the illness even though it’s complex and impossible to understand.
But when someone gets a diagnosis of cancer, their community rallies for them. They call them a fighter. They support them and their family. But for me it’s like the play has silently ended prematurely and I quietly slipped into the background, never to be seen again, but no one noticed much.
My family and I are not getting real world community support, instead much of the opposite: a total lack of understanding and being shamed.
I’m not the only one suffering from this illness… my husband and my children also have to adjust. How does my little one not internalize the fact that mummy can rarely play now? And my husband – he suddenly has the weight of the world on his shoulders. And the teenager… I’m sure he cares too. Maybe.
In some ways I think it’s harder on my family than on myself.
I’m already in-and-out of a place of acceptance and trying to ensure a decent future for them either way. But I’m not sure how they feel and they can’t really confide in me about it without making me feel worse. But they also don’t have anyone to rally around them and ensure them everything will be okay.
Can I pay someone to care?
Ya know, assuming I have the money.
There are no family support groups that I can find for this. Or councilors who will see us and actually understand the illness and it’s implications. Without that I’m not sure it would be useful. “Erica, why can’t your do the dishes and wash your hair after playing with your son?” I don’t need more people to defend myself against.
I am working with an advocacy group, Long Covid Families, and we are trying to help build the supports that people like us so desperately need. It gives me hope and purpose.
This world is not disability friendly
I wrote a marriage councilor who we used to see and explained the situation. I said that I was disabled and would need telehealth. He didn’t get it, and 3 times he wrote me back saying I need to come in person.
He wants me to at least “work out doing the first session in person.” This building only has stairs, and he’s on the 3rd floor, forget the crash, I cannot even get to his office. And clearly he’s not going to be the type of help we need anyways.
How ya doing?
In the beginning, when people would ask how I am, I would try to tell them about the illness and what I have learned even though it’s so confusing and difficult.
A few people have totally ignored me, they literally just didn’t respond. Some have changed the subject.
Some have made harsh statements, some simply misguided:
“She better not get a wheelchair.”
“Sounds like typical COVID anxiety”
“You’re giving it power by talking about it.”
“Do you think keeping a symptom tracker is focusing too much on what’s going wrong?”
“Have you tried yoga, vitamins, drinking more water, etc. etc. etc?”
“Don’t give up seeing doctors! There has to be treatment!”
A few special gems of people do ask questions about the illness, even more amazing a couple have done their own research. A few continue to check in and tell me they love me and that they are sorry.
I’m not sure what exactly it is I even expect from people.
Not victim blaming is a good place to start.
I no longer answer how I am doing truthfully, if even at all.



